How to Integrate Peptide Therapy With Your Hormone Optimization Protocols
How to Integrate Peptide Therapy With Your Hormone Optimization Protocols
![[HERO] How to Integrate Peptide Therapy With Your Hormone Optimization Protocols](https://cdn.marblism.com/QMokyCltQ6R.webp)
The landscape of modern longevity medicine has evolved significantly, shifting from the basic treatment of endocrine deficiencies to a more sophisticated model of comprehensive physiological optimization. While traditional Hormone Replacement Therapy (HRT) has long served as the cornerstone for managing age-related hormonal decline, the integration of peptide therapy represents a revolutionary advancement in restorative clinical practice. Specifically, the strategic combination of exogenous hormones with targeted signaling peptides allows healthcare providers to address the complexities of the human endocrine system with unprecedented precision. By leveraging these synergistic pathways, practitioners can achieve superior clinical outcomes that extend far beyond the capabilities of monotherapy.
How Does Peptide Therapy Complement Traditional Hormone Replacement?
The primary distinction between traditional HRT and peptide therapy lies in their fundamental mechanism of action within the human body. Traditional hormone replacement involves the direct administration of exogenous hormones, such as testosterone, estrogen, or progesterone, to replace levels that have diminished due to aging or pathology. While this approach is highly effective at raising serum hormone concentrations, it frequently triggers a negative feedback loop that suppresses the body’s own endogenous production. Furthermore, chronic reliance on exogenous hormones can lead to the desensitization of receptor sites over time, necessitating higher doses or additional interventions to maintain the desired therapeutic effect.
Conversely, peptide therapy functions as a targeted signaling mechanism that encourages the body to restore its own innate hormonal balance. Growth Hormone Releasing Peptides (GHRPs) and Growth Hormone Releasing Hormones (GHRHs) do not replace growth hormone; instead, they stimulate the pituitary gland to increase its natural secretion of the hormone. When integrated into a broader hormone optimization protocol, peptides act as a physiological bridge, maintaining the integrity of the endocrine signaling axis while exogenous hormones provide the necessary foundational support. This multifaceted approach ensures that the patient’s biological systems remain active and responsive, ultimately leading to a more sustainable and vibrant state of health.
Why is Pituitary Health Essential for Long-Term Endocrine Success?
The pituitary gland, often referred to as the "master gland," plays a critical role in orchestrating the complex dance of the endocrine system. As individuals age, the pituitary's output of vital hormones, particularly growth hormone, begins to decline: a process known as somatopause. Traditional HRT protocols often overlook the health of the pituitary gland, focusing instead on downstream hormones like testosterone or thyroid markers. However, failing to address the underlying signaling decline at the pituitary level can result in a metabolic plateau where the patient feels "better" but does not reach their full potential for tissue repair, fat metabolism, and cognitive clarity.
Specifically, peptides like Ipamorelin are instrumental in preserving and enhancing pituitary function within a hormone optimization framework. Unlike older generations of secretagogues, Ipamorelin is highly selective and does not significantly impact cortisol or prolactin levels, making it an ideal candidate for long-term integration. By providing a pulsatile stimulus to the pituitary gland, these peptides mimic the body’s natural biorhythms, promoting the release of growth hormone in a manner that is both safe and effective. Moreover, supporting the pituitary gland through peptide therapy helps to preserve the sensitivity of various hormonal axes, ensuring that the patient remains responsive to the broader optimization protocol for years to come.
What Role Do CJC-1295 and Ipamorelin Play in Growth Hormone Optimization?
The combination of CJC-1295 and Ipamorelin is widely considered the gold standard for growth hormone optimization in the longevity space. CJC-1295 is a synthetic GHRH analog that increases plasma growth hormone levels by extending the half-life of the signal, whereas Ipamorelin acts as a potent GHRP that triggers the actual release of the hormone from the pituitary. When administered together, these two peptides provide a powerful synergistic effect that dramatically enhances the body’s regenerative capacity. Specifically, this combination promotes lean muscle mass development, accelerates lipolysis, and improves overall bone density, which are critical factors for patients undergoing hormone optimization.
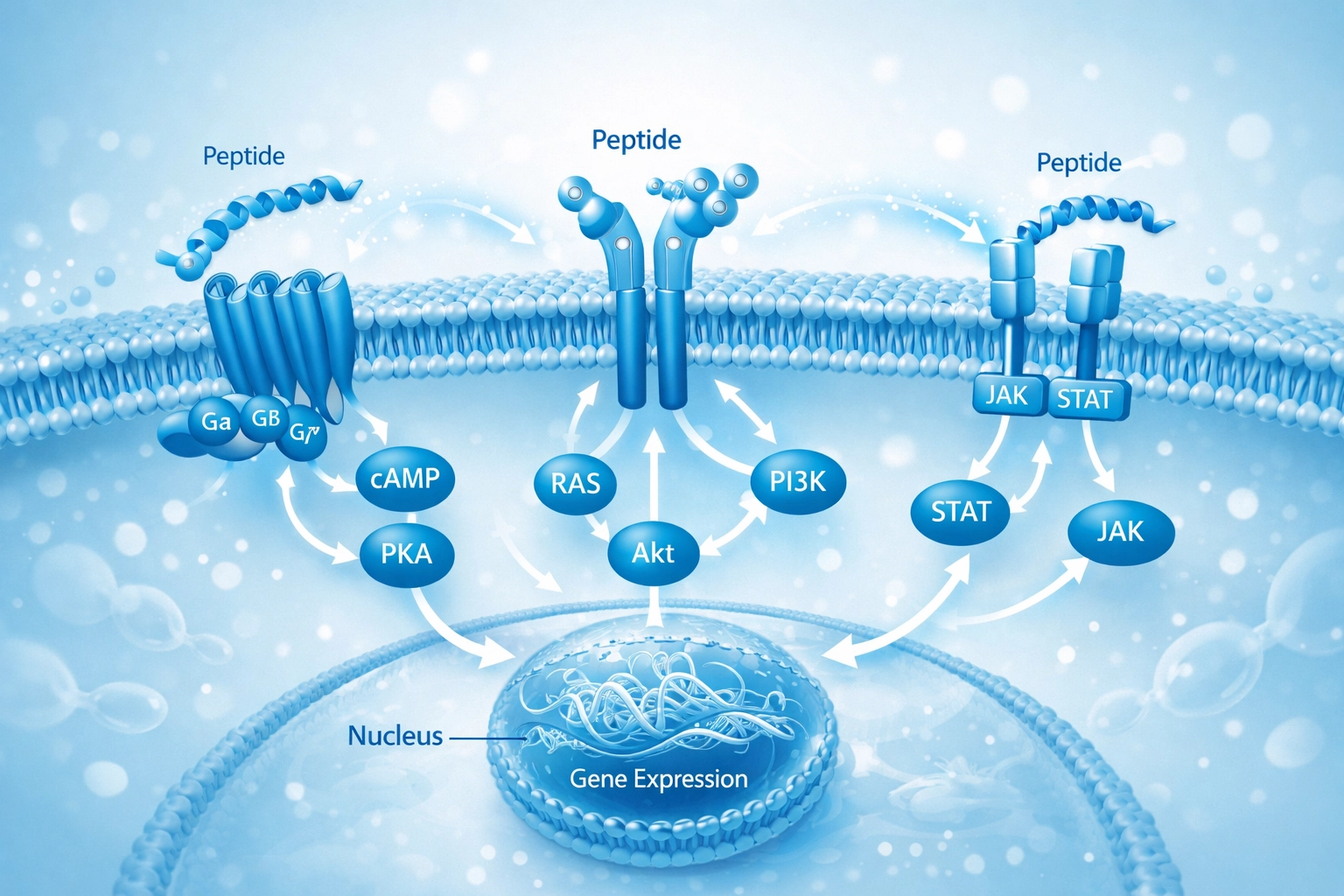
Furthermore, the integration of these peptides into a traditional HRT protocol can significantly enhance the subjective well-being of the patient. While testosterone replacement may improve libido and energy, the addition of growth hormone secretagogues often results in better sleep quality, improved skin elasticity, and faster recovery from physical exertion. Specifically, for healthcare professionals, utilizing the high-purity formulations available at Biomed Peptides ensures that the clinical results are predictable and consistent. Whether utilizing injectable or oral formulations, the goal remains the same: to create a robust hormonal environment that supports the patient’s aesthetic and functional goals simultaneously.
How Can BPC-157 and TB-500 Enhance Systemic Recovery?
While growth hormone secretagogues focus on endocrine signaling, other peptides like BPC-157 and Thymosin Beta-4 (TB-500) provide essential systemic support that complements hormone therapy. Hormone optimization often leads to increased physical activity and higher intensity workouts, which can put additional strain on the musculoskeletal system. BPC-157, a pentadecapeptide derived from human gastric juice, is renowned for its ability to accelerate the healing of tendons, ligaments, and muscle tissue. By modulating the angiogenic process and increasing the expression of growth factor receptors, BPC-157 ensures that the body can keep up with the metabolic demands of an optimized hormonal state.

Additionally, the use of the "Wolverine Blend": a combination of BPC-157 and TB-500: offers a comprehensive approach to managing systemic inflammation and tissue repair. TB-500 works by upregulating actin, a protein vital for cell migration and wound healing, which works in tandem with the regenerative properties of BPC-157. For a patient on a testosterone or estrogen optimization protocol, these peptides act as a "safety net," reducing the risk of injury and ensuring that the physical gains achieved through hormone therapy are not hindered by chronic pain or inflammation. This level of systemic support is what differentiates a standard wellness clinic from a high-performance longevity practice.
What Are the Metabolic Advantages of Integrating Mitochondrial Peptides?
Beyond the traditional anabolic and androgenic axes, the integration of metabolic peptides like MOTS-c offers a unique pathway for optimizing cellular energy and insulin sensitivity. MOTS-c is a mitochondria-derived peptide that regulates metabolic homeostasis and has been shown to improve exercise capacity and glucose metabolism. In patients undergoing hormone optimization, metabolic health is often the "missing piece" that prevents optimal body composition. By incorporating MOTS-c into a protocol, practitioners can target the mitochondrial level of the cell, enhancing the efficiency with which the body utilizes the hormones being optimized.

Moreover, the use of metabolic peptides can be particularly beneficial for patients who struggle with weight management despite having optimized hormone levels. For instance, combining Cagrilintide and GLP-1 agonists with traditional HRT and secretagogues creates a multi-layered approach to metabolic health that addresses appetite, insulin signaling, and growth hormone production all at once. This comprehensive strategy ensures that the patient’s metabolism is working in harmony with their endocrine system, leading to sustainable fat loss and improved cardiovascular markers. The future of hormone optimization undoubtedly lies in this type of multi-peptide integration.
Clinical Implementation: Monitoring and Sourcing Purity
For healthcare providers, the successful integration of peptide therapy requires diligent monitoring and a commitment to utilizing the highest quality compounds. Comprehensive baseline lab testing, including IGF-1, fasting insulin, and a complete hormone panel, is essential for tailoring a protocol to the individual needs of the patient. Regular follow-up testing allows for the adjustment of dosages and the fine-tuning of the peptide-hormone synergy. Additionally, practitioners must prioritize sourcing from reputable manufacturers that provide third-party testing and Certificates of Analysis (COAs) to ensure the purity and potency of the peptides being administered.

Specifically, Biomed Peptides offers a comprehensive range of injectable and oral formulations designed for the modern longevity practice. From high-purity Thymosin Alpha-1 for immune support to the latest in metabolic signaling, having access to reliable, USA-manufactured peptides is paramount for clinical success. By partnering with a dedicated supplier, healthcare professionals can focus on the art of medicine, knowing that the tools they are using meet the rigorous standards of the pharmaceutical and healthcare industry.
The Future of Integrated Endocrine Medicine
The integration of peptide therapy with hormone optimization protocols represents a profound shift toward a more holistic and biologically harmonious approach to human health. By combining the foundational power of HRT with the precise signaling of peptides, practitioners can unlock a level of vitality that was previously thought to be unattainable. As research continues to uncover new peptides and their roles in human physiology, the potential for personalized medicine will only expand. Healthcare providers who embrace these advancements today will lead the charge in the future of regenerative medicine, offering their patients a path to longevity that is truly transformative.

